If you or someone you know has been diagnosed with multiple sclerosis (MS), you probably have many questions. Understanding MS is essential to effective management and improving quality of life. Follow along as we answer some of the most commonly asked questions about MS, providing valuable insight and information. Given how the symptoms of multiple sclerosis can often be misdiagnosed, it’s helpful to research this information online before consulting a doctor.
What is MS?
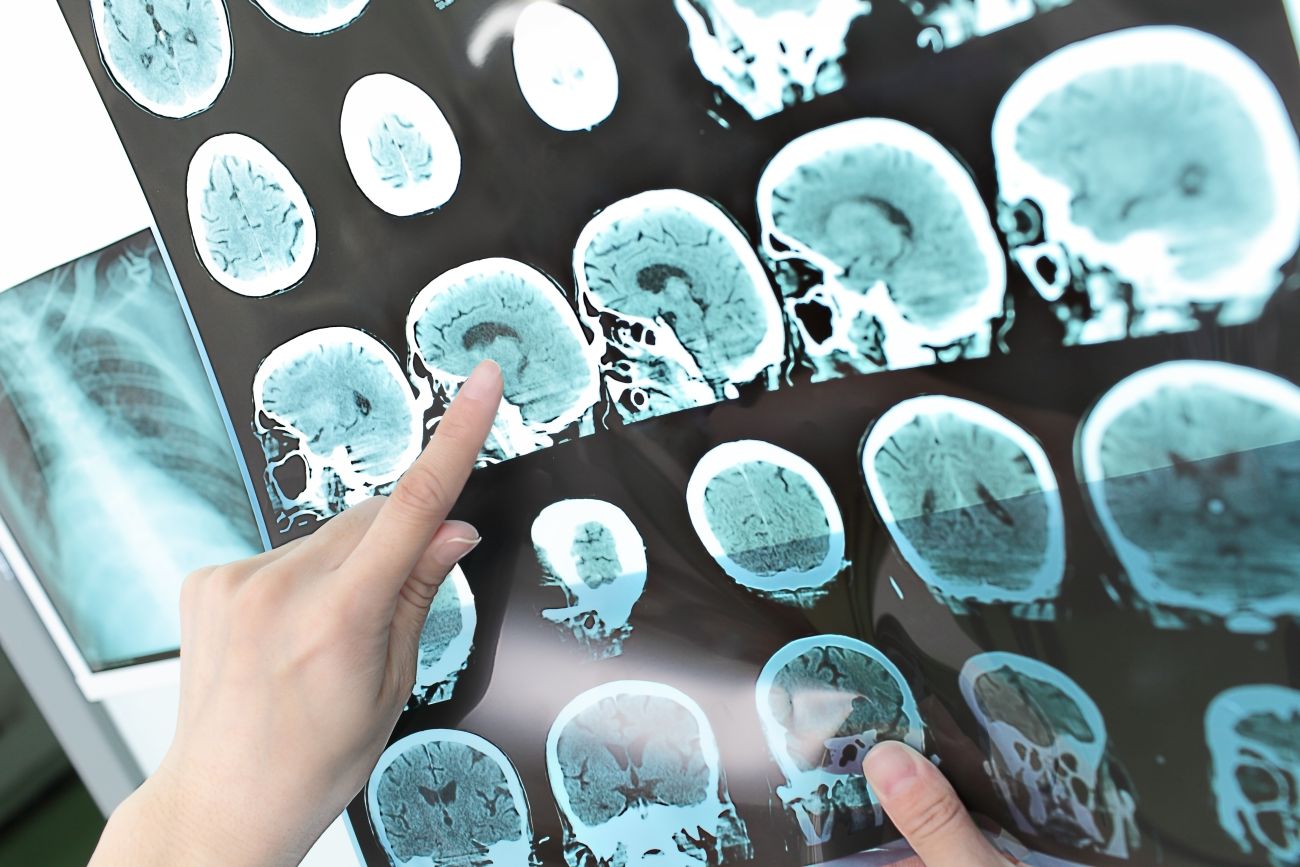
MS is a chronic disease that affects the brain and spinal cord, or central nervous system (CNS). It is characterized by inflammation and the erroneous destruction of the protective covering of nerves (myelin) by our own body.
This destruction of myelin interrupts the flow of information within the brain and between the brain and body. Its course is often progressive, insidious, and unpredictable, leading to some level of disability.
Who is at Risk for Multiple Sclerosis?
Although the exact cause of MS remains elusive, there are well-established risk factors for this chronic neurological disease.
Risk factors for MS include:
- Age: Adults between 20 and 40 are more susceptible to the disease.
- Gender: Females have double the risk as compared with males.
- Smoking: Smokers have double the risk as compared with non-smokers.
- Where You Live: Risk of MS increases the further away you live from the equator
- Certain Infections: For instance, Epstein-Barr virus, the cause of “mono”, can increase your risk of having MS.
- Having Another Autoimmune Disease: Having lupus or rheumatoid arthritis can increase your risk of having MS.
- Your Family History: Having a family member with MS can increase your risk of having MS.
What Are The First Signs of MS?
The signs and symptoms of MS can be insidious and may often be misread or minimized. The very first signs of MS are highly variable. They may include:
- Tingling and numbness;
- Fatigue;
- Visual disturbances;
- Spasticity, and;
- Dizziness.
Other early symptoms of MS may be more telling or bothersome. They include:
- Bladder and bowel issues;
- Sexual problems;
- Problems with memory and thinking, and;
- Emotional issues.
What Does MS Pain Feel Like?
Pain typically accompanies MS. This pain can be either neuropathic or musculoskeletal. Neuropathic pain comes directly from damage to nerves in the CNS. Many describe it as burning, stabbing, sharp, and even squeezing.
Musculoskeletal pain results from spasticity or muscle weakness. It can alter gait and mobility, further compounding the pain. Regardless of their cause, both types of pain can be acute or chronic, as well as intermittent.
What Are The Different Types of MS?
Neurologists take care of most individuals diagnosed with MS. These MS specialists categorize the disease into the following types:
- Clinically isolated syndrome (CIS)
- Relapsing-remitting MS (RRMS), the most common type of MS as it makes up 85 percent of cases
- Secondary progressive MS (SPMS), which usually develops from RRMS
- Primary progressive MS (PPMS)
Unfortunately, there is no way to predict the course of the disease with any certainty.
How is MS Treated?
Currently there is no cure for MS. However, there are treatment options that can help ease symptoms and slow down or even halt disease progression. The mainstays of MS treatment are prescription “disease-modifying” medications that can be swallowed, injected, or infused. Other treatments are symptom-specific, such as medicines, physical therapy, occupational therapy, and/or speech therapy.
Complementary and alternative medicine (CAM) therapies have recently gained mainstream popularity for the treatment of many medical conditions, including MS. CAM therapies include the use of herbs and supplements, yoga, and acupuncture.
What is the Life Expectancy of a Person with MS?
The average life expectancy of someone diagnosed with MS is almost seven years less than someone who does not have the disease.
Over the years, the life expectancy of those with MS has improved. This can be attributed to advances in treatment and care as well as more attention to lifestyle modifications.
Can You Die from MS?
MS itself is very rarely fatal. If death occurs, it is primarily due to complications or other co-existing medical conditions, such as heart disease, cancer, diabetes, and high blood pressure.
An MS diagnosis has the potential to severely decrease your quality of life. The decrease in quality of life is mostly a function of complications of the disease, leading to disability.
Can I Stop MS From Progressing?
Although MS is not always progressive, you have the best chance of stopping the progression of the disease with early diagnosis and treatment. In addition to regularly taking your prescribed medications, you should assemble a health care team that you trust and are comfortable with.
It is this combination that has the potential to stop — or at least slow — MS in its tracks.
Does MS Cause Paralysis?
The odds of MS causing permanent paralysis are extremely low, so much so that most experts would answer “No” to the above question.
The National Multiple Sclerosis Society estimates that two-thirds of MS patients maintain the ability to walk through assistive aids.
Learn More About Multiple Sclerosis Today!
MS can be challenging to navigate, but knowledge is your most powerful tool. To gain a deeper understanding and find answers to the most commonly asked questions about MS, we encourage you to continue exploring online resources. Your journey to comprehending and managing MS starts with a simple online search, and you’re not alone in your pursuit of knowledge.